Synthetic stem cells offer benefits of natural stem cells without the risks
January 13, 2017
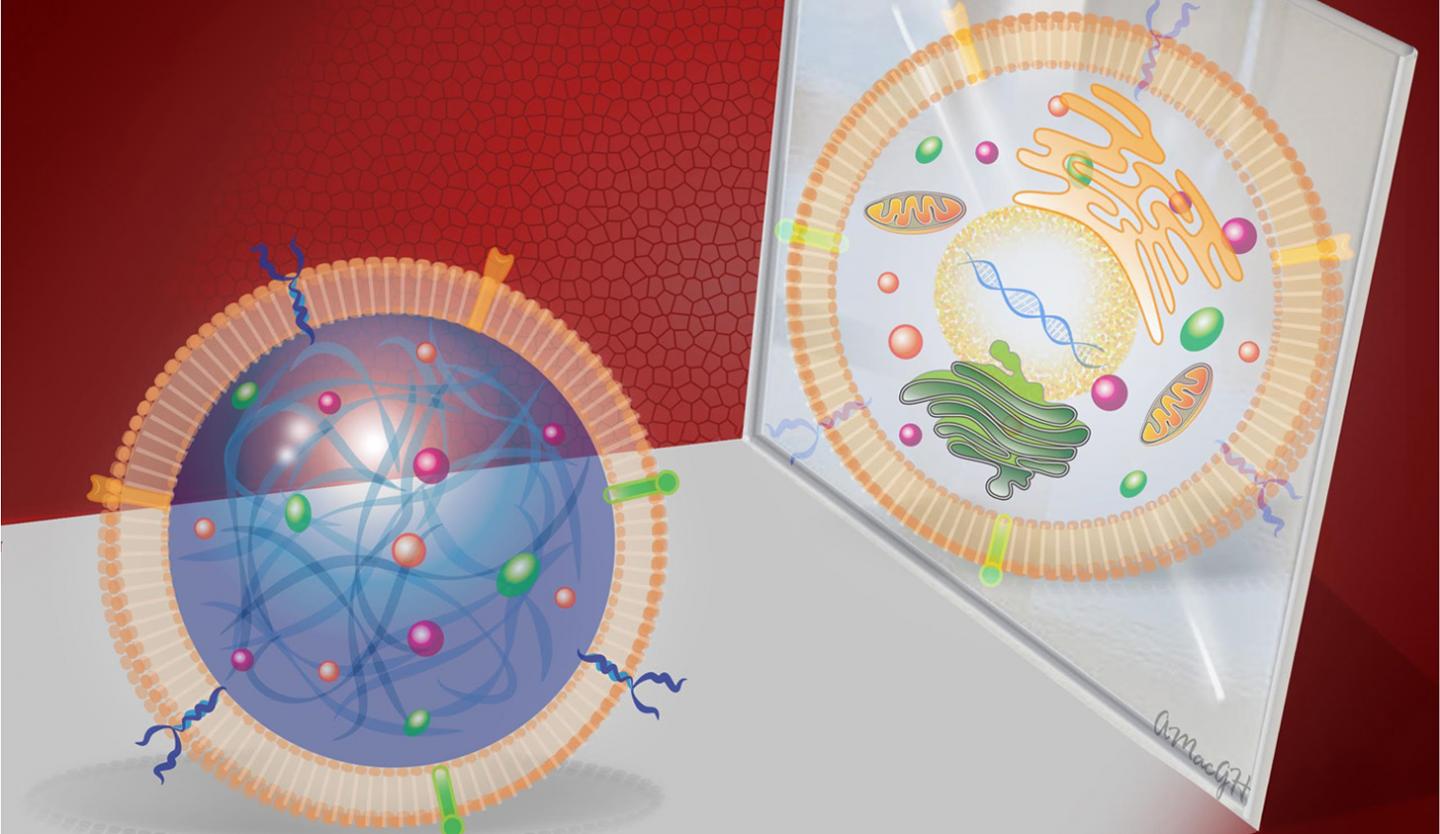
A synthetic cardiac stem cell (left) mirroring a real cardiac stem cell (right), offering therapeutic benefits without the associated risks (credit: Alice Harvey/NC State University)
Scientists have created the first synthetic version of a cardiac stem cell, offering therapeutic benefits comparable to those from natural stem cells — but without the risks and limitations, according to researchers from North Carolina State University, the University of North Carolina at Chapel Hill, and First Affiliated Hospital of Zhengzhou University in China.
The newly created “synthetic stem cells” (not actual stem cells — not even cells — just clever mimics) cannot replicate. That means they could reduce some of the risks associated with natural stem-cell therapies — including tumor growth and immune rejection. The synthetic stem calls would also avoid the fragility of natural stem cells, which require careful storage and a multi-step process of typing and characterization before they can be used.
Simulating cardiac stem cells with synthetic stem cells: a cargo-shell strategy
In an in vitro (test tube) experiment described in an open-access paper in Nature Communications, the scientists created synthetic “cell-mimicking microparticles” (CMMPs) and tested them on a mouse model with myocardial infarction.
The scientists found that the CMMPs’ ability to bind to cardiac tissue and promote growth after a heart attack was comparable to that of cardiac stem cells. But unlike cardiac (and other) natural stem cells, the synthetic stem cells have better preservation stability, and the technology is also generalizable to other types of stem cells, according to the researchers.
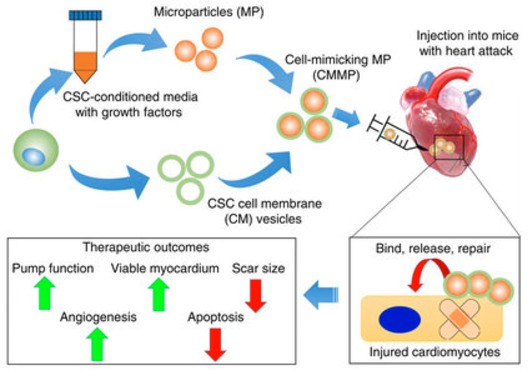
A cargo-and-shell strategy. The therapeutic potential of CMMPs was successfully tested in tissue repair of a mouse model of myocardial infarction. To create the synthetic stem cell, a microparticle (MP) was first fabricated from PLGA, or poly(lactic-co-glycolic acid) — a biodegradable, biocompatible polymer that serves as a dissolvable carrier. The MP contained conditioned media and growth factors* (the “cargo”) from cardiac stem cells (CSC) in its polymeric core — forming a synthetic cell-mimicking microparticle (CMMP). To prevent an immune reaction, the researchers also cloaked the CMMP with a coating from the cardiac stem-cell membrane (forming the “shell”). (credit: Junnan Tang et al./Nature Communications)
“The synthetic cells operate much the same way a deactivated vaccine works,” explains research-team leader Ke Cheng, associate professor of molecular biomedical sciences at NC State, associate professor in the joint biomedical engineering program at NC State and UNC, and adjunct associate professor at the UNC Eshelman School of Pharmacy. “[The synthetic cells’] membranes allow them to bypass the immune response, bind to cardiac tissue, release the growth factors, and generate repair, but they cannot amplify [and thus risk out-of-control growth, leading to tumors] by themselves. So you get the benefits of stem cell therapy without risks.”
Multiple stem-cell types and organs
The synthetic stem cells are also much more durable than human stem cells, they can tolerate harsh freezing and thawing, and they don’t have to be derived from the patient’s own cells, the researchers note.
“Although our first application targeted the heart, the CMMP strategy represents a platform technology that can be applied to multiple stem cell types and the repair of various organ systems,” the authors state in the paper.
The work was funded in part by the National Institutes of Health, NC State Chancellor’s Innovation Fund, and University of North Carolina General Assembly Research Opportunities Initiative grant.
* Stem-cell therapies work by secreting “paracrine factors,” including proteins and genetic materials, that aid damaged tissue in repairing itself.
Abstract of Therapeutic microparticles functionalized with biomimetic cardiac stem cell membranes and secretome
Stem cell therapy represents a promising strategy in regenerative medicine. However, cells need to be carefully preserved and processed before usage. In addition, cell transplantation carries immunogenicity and/or tumorigenicity risks. Mounting lines of evidences indicate that stem cells exert their beneficial effects mainly through secretion (of regenerative factors) and membrane-based cell-cell interaction with the injured cells. Herein, we fabricated a synthetic cell-mimicking microparticle (CMMP) that recapitulates stem cell functions in tissue repair. CMMPs carries similar secreted proteins and membranes as genuine cardiac stem cells do. In a mouse model of myocardial infarction, injection of CMMPs leads to preservation of viable myocardium and augmentation of cardiac functions similar to cardiac stem cell therapy. CMMPs (derived from human cells) do not stimulate T cells infiltration in immuno-competent mice. In conclusion, CMMPs act as “synthetic stem cells” which mimic the paracrine and biointerfacing activities of natural stem cells in therapeutic cardiac regeneration.
