These fast, low-cost medical technologies will replace ultrasound and X-rays for specific uses
September 8, 2017
Smartphone instant heart diagnosis (credit: Caltech)
A radical software invention by three Caltech engineers promises to allow your smartphone camera* to provide detailed information about a critical measure of your heart’s health: the “left ventricular ejection fraction” (LVEF) — the amount of blood in the heart that is pumped out to the blood system with each beat. This figure is used by physicians as a base for diagnostic and therapeutic decisions.
You’ll simply hold your phone up to your neck for a minute or two.
In an experiment, the technique was found to be as accurate as a 45-minute echocardiography scan, which currently requires a trained technician operating an expensive ultrasound machine.
The smartphone technique measures how much the carotid artery displaces the skin of the neck as blood pumps through it. In a normal heart, the LVEF measure ranges from 50 to 70 percent. When the heart is weaker, less of the total amount of blood in the heart is pumped out with each beat, and the LVEF value is lower.
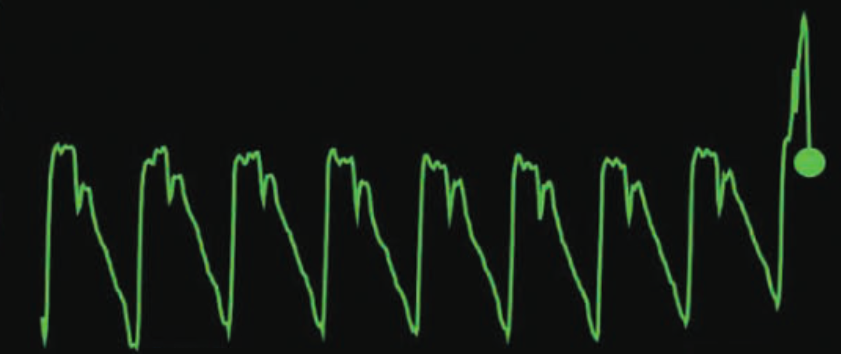
Carotid arterial waveform captured using an unmodified iPhone 5S camera by placing the iPhone camera over the carotid pulse (credit: Niema M. Pahlevan et al./Critical Card Medicine)
To test the app, clinical trials were conducted with 72 volunteers between the ages of 20 and 92 at an outpatient magnetic resonance imaging (MRI) facility. MRI is the gold standard in measuring LVEF but is seldom used clinically due to its high cost and limited availability. The measurements made by smartphone had a margin of error of ±19.1 percent compared with those done in an MRI. By way of comparison, the margin of error for echocardiography is around ±20.0 percent.
“This has the potential to revolutionize how doctors and patients can screen for and monitor heart disease, both in the U.S. and the developing world,” says Caltech’s Mory Gharib, the Hans W. Liepmann Professor of Aeronautics and Bioinspired Engineering and senior author of a paper on the study in the July issue of the Journal of Critical Care Medicine.
The researchers have founded a start-up named Avicena, LLC that has licensed this technology and will market the app. They also plan to use this approach to diagnose heart-valve diseases, like aortic stenosis and coronary artery blockage.
* For the study, the team used an iPhone 5, but they say any smartphone with a camera will work.
Seeing through the body
University of Edinburgh and Heriot-Watt University researchers have used a near-infrared camera to see through the chest to track the location of a fiber-optic endomicroscope (a long flexible tube with a light on the end) — replacing X-rays.
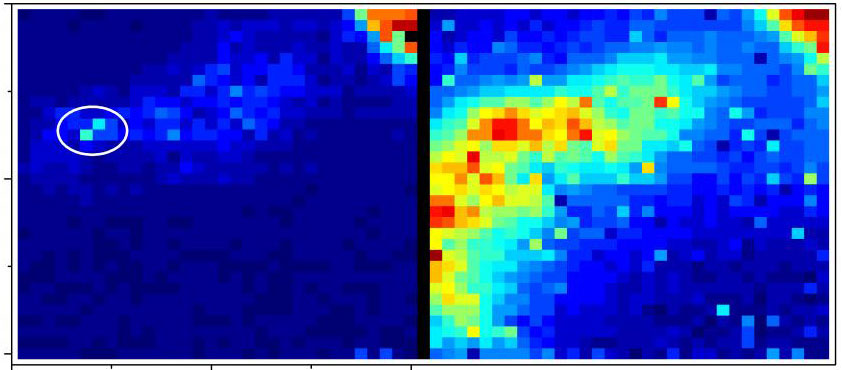
A “time-of-flight” camera detects light emitted from an endoscope in sheep lungs. Left: light emitted from the tip of the endoscope, revealing its precise location in the lungs. Right: an image using a conventional camera, with light scattered through the structures of the lung. (credit: Proteus)
Near-infrared light can readily pass through the body, but much of it scatters or bounces off tissues and organs rather than traveling straight through — making it nearly impossible to get a clear picture of where an object is in the body. So this camera uses a “time-of-flight” system: It calculates the distance to the endomicroscope light based on the time it takes individual photons to arrive directly (ignoring scattered photons, which take longer). That’s similar to how this camera can see an object around a corner.
The technology is so sensitive it can detect the miniscule amount of light that passes through 20 centimeters (about 8 inches) of the body’s tissue.
The research is described in an open-access paper in the journal Biomedical Optics Express.
Abstract of Noninvasive iPhone Measurement of Left Ventricular Ejection Fraction Using Intrinsic Frequency Methodology
Objective: The study is based on previously reported mathematical analysis of arterial waveform that extracts hidden oscillations in the waveform that we called intrinsic frequencies. The goal of this clinical study was to compare the accuracy of left ventricular ejection fraction derived from intrinsic frequencies noninvasively versus left ventricular ejection fraction obtained with cardiac MRI, the most accurate method for left ventricular ejection fraction measurement.
Design: After informed consent, in one visit, subjects underwent cardiac MRI examination and noninvasive capture of a carotid waveform using an iPhone camera (The waveform is captured using a custom app that constructs the waveform from skin displacement images during the cardiac cycle.). The waveform was analyzed using intrinsic frequency algorithm.
Setting: Outpatient MRI facility.
Subjects: Adults able to undergo MRI were referred by local physicians or self-referred in response to local advertisement and included patients with heart failure with reduced ejection fraction diagnosed by a cardiologist.
Interventions: Standard cardiac MRI sequences were used, with periodic breath holding for image stabilization. To minimize motion artifact, the iPhone camera was held in a cradle over the carotid artery during iPhone measurements.
Measurements and Main Results: Regardless of neck morphology, carotid waveforms were captured in all subjects, within seconds to minutes. Seventy-two patients were studied, ranging in age from 20 to 92 years old. The main endpoint of analysis was left ventricular ejection fraction; overall, the correlation between ejection fraction–iPhone and ejection fraction–MRI was 0.74 (r = 0.74; p < 0.0001; ejection fraction–MRI = 0.93 × [ejection fraction–iPhone] + 1.9).
Conclusions: Analysis of carotid waveforms using intrinsic frequency methods can be used to document left ventricular ejection fraction with accuracy comparable with that of MRI. The measurements require no training to perform or interpret, no calibration, and can be repeated at the bedside to generate almost continuous analysis of left ventricular ejection fraction without arterial cannulation.
Abstract of Ballistic and snake photon imaging for locating optical endomicroscopy fibres
We demonstrate determination of the location of the distal-end of a fibre-optic device deep in tissue through the imaging of ballistic and snake photons using a time resolved single-photon detector array. The fibre was imaged with centimetre resolution, within clinically relevant settings and models. This technique can overcome the limitations imposed by tissue scattering in optically determining the in vivo location of fibre-optic medical instruments.
